Disclosure: Our Family Lifestyle is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to amazon.com.
You know how every mom who has went through labor and delivery has a birth story. They all come out the second you announce you’re pregnant, right?! “When I was in labor…”
Well, I have found that with my hysterectomy, I definitely wasn’t told enough. Perhaps it’s the times we’re living in, meaning I wasn’t really around anyone to be told.
But, even when I told my Facebook friends, I still only received well wishes. Which, I’m not complaining about. I just didn’t have any one telling me about their hysterectomies.
In fact, it was after I began sharing my hysterectomy recovery journey on Instagram when other women started sharing their stories.
That was when I discovered others had experienced what I had. They had shared my pain. They knew my struggles.
Well, I’m going to try and do you a solid today and share some of the post-hysterectomy challenges with you so you’ll be prepared should you need it.
If that’s what led you to this post today, then, get ready, we’re going to jump right in.
Gas Pain
My one and only pain for the first week post-surgery was GAS! Seriously!
No one told me about this. Even before I left the hospital 24 hours post-surgery, as I was trying to understand why my shoulders hurt each time I stood up, I was lost as to why.
Therefore, I asked my doctor.
He explained how they use gas to open up the space in your stomach so they can operate. The pain is from the gas “attaching” to a nerve in my diaphragm and traveling up to my shoulder.
He said that even though the nurses had been giving me a heating pad for the pain, it’s hard to manage because that’s not the real point of the pain.
All I know is that the four “stab wounds” in my stomach never gave me any real pain; only the gas did.
My stomach was hard and distended for over a week! And the gas medication (prescription strength Gas-X) didn’t seem to offer me much relief.
Hopefully you have better luck.
Percocet
When my doctor and I talked just before they came to take me back for surgery, I told him I had a migraine.
(Y’all, my period was over 45 days late and chose THAT morning to start! I told it I got the last laugh because I was kicking my uterus out!)
Anyways, he asked me how often I got migraines and how bad they were. He then decided to switch my post-op medication therapy to include Percocet.
Now, side note, I barely take Tylenol. I’m not big of taking medications unless they’re absolutely necessary.
That being said, taking an Opioid was a big deal for me. We read all of the possible side effects and knew what to watch for.
I have to assume it did its job, because, other than the gas, I really didn’t have any other pain.
But, what I was NOT prepared for was the detox.
I’ve never been addicted to anything, don’t take medications regularly, and didn’t have much to go off of.
Seven days post-hysterectomy, we started weaning off the Percocet. The next morning I woke up with a slight headache.
This seemed strange considering how much medication I was on and I had not experienced a headache since the surgery.

As the day progressed, I felt like I was dragging, but I was still only a week into recovery.
When I went I shower that night, I had to hurry through the process because I was too cold.
By the time I climbed into bed, my teeth were chattering and goosebumps covered my body. I could not get warm.
I had been telling Colby since late evening I felt like my face was burning. He insisted I didn’t have a fever while I insisted I did.
By this point, I was adamant about checking my temperature to be sure. Unfortunately though, we had sent our thermometer home with our daughter recently to monitor a low-grade temperature her toddler was having.
So, Colby began tearing apart the house looking for another thermometer. We should have two more. Couldn’t find either; of course. (We’ve since ordered a new one –linked above– for our home).
I was desperate, so I asked if anyone was awake at 1am in our neighborhood Facebook group. I just desperately wanted to check my temperature to prove I wasn’t insane.
Luckily, someone was up and willing to loan us a thermometer. It didn’t take much to confirm I had a fever.
In fact, I had a fever and chills. Flu-like symptoms. As well as paranoia and a few other signs that signaled this was a result of detoxing.
This was the absolute worst night of my recovery.
It took me quite a while to fall asleep. Colby sat up staring at me as I struggled to get and stay warm, stopped taking crazy stuff, and drift off to sleep.
By the time I woke hours later, my bed beneath me was soaked with sweat. My gown and hair both drenched signaling that my fever had broken.
Although feeling a bit groggy and run down the following day, I seemed to have made it past the hump of the detox.
Honestly, past the hump of my recovery overall.
Other than unrelated fall onto our ceramic tile floor (doing perhaps the most grandmother thing ever: trying to find for my granddaughter), my healing has been going well.
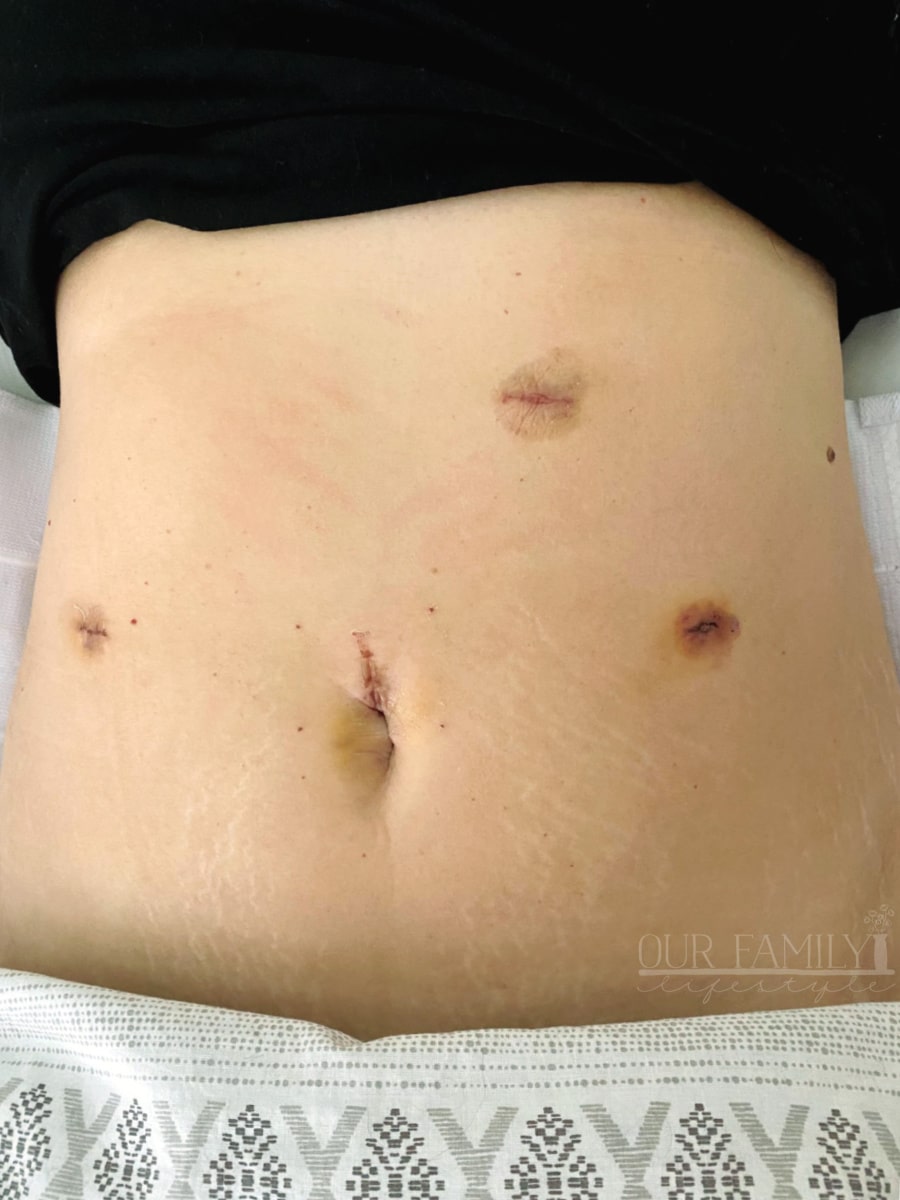
Surgical Glue
The only remaining discomfort is with the actual stab wounds (as I call them).
I had a robotic hysterectomy that left four small cuts on my abdomen. Each one was sealed with surgical glue.
Another side note, I’ve never had a major surgery like this before and have also never had stitches.
Therefore, I wasn’t sure what to expect as far as the glue either. Before leaving the hospital I was told:
- no baths
- pat don’t rub to dry
- don’t pull at the glue
Everything else was pretty much common sense and I’ve had no issues with beyond some itching as it begins to dry.
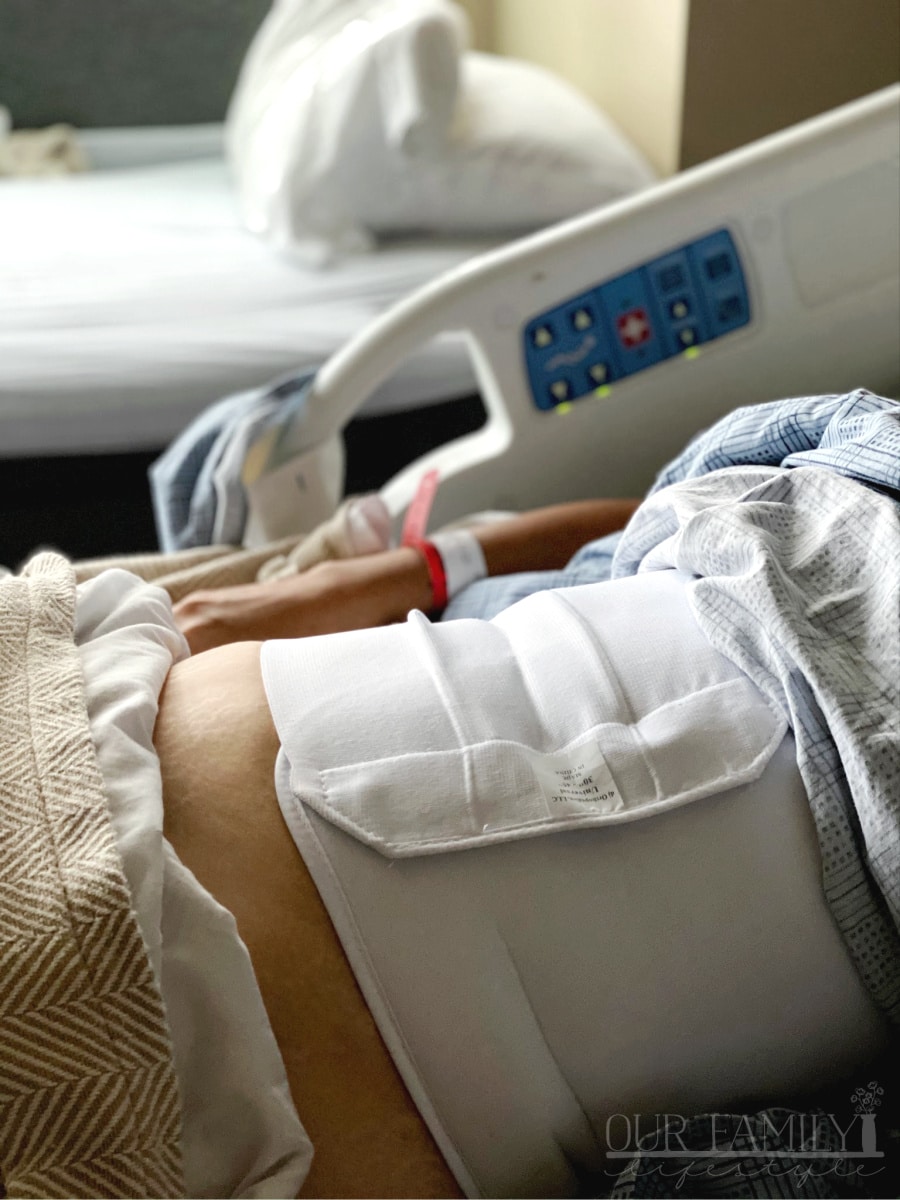
Abdominal Binder
Again, with nothing to go on with my previous experience, I didn’t know about the abdominal binder. It’s basically a wide compression belt.
My nurse said it often helps relieve some of the pain after surgery, so I decided to wear it. In fact, the binder can also (per Healthline):
- increase circulation at your surgical site to promote healing and decrease swelling
- make physical activity more comfortable
- strengthen abdominal muscles
I have no baseline to go on for the physical benefits, but I can tell you it became a security binder for me.
I felt safer wearing it. It kept me from accidently swiping something close to my wounds, kept Colby from unknowingly touching them at night, and kept my clothes from rubbing on the glue.
It may seem like a small thing, but it truly made a big difference for me.
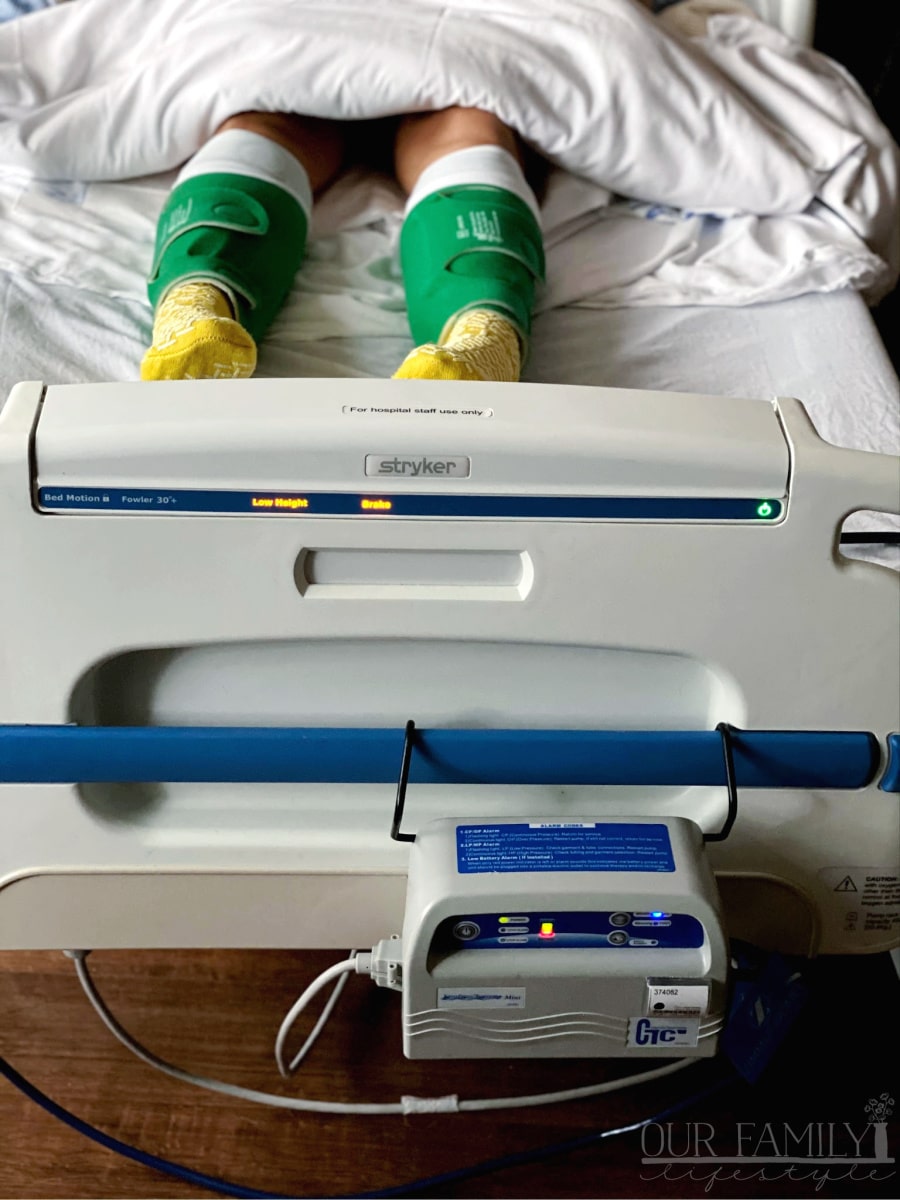
Intermittent Pneumatic Compression
This one I have to mention was in the hospital only, but made sleeping so much easier for some reason: intermittent pneumatic compression (IPC).
Basically, it’s leg cuffs (similar to blood pressure cuffs) that are wrapped around your calves to fill with air and squeeze intermittently.
The medical purpose of them is to increase blood flow to help prevent blood clots.
They felt so good to me when I was sleeping at the hospital that I was very sad to leave them behind.
Tomorrow I will officially be two weeks post-hysterectomy and feel like I’m back to about 97%.
The biggest thing though?
I HAVE NOT HAD ANY BLEEDING!
Even post-surgery, while still in the hospital, I only saw a slight tinge of blood the first few trips to the bathroom. Nothing since.
You may or may not understand how life-changing this will be for me! I am still amazed every day by it.
I’ve been very transparent on how much abnormal bleeding I’ve experienced over the past three years. It’s been a very challenging health journey.
The ovarian cysts, fibroids, polyps, biopsies, anemia… all of it has taken it’s toll on my mental health. As if my anxiety needed more to stress over.
Surgical Note:
After the surgery, my doctor confirmed (and gave me photos for hard evidence) that I had a large cyst on one fallopian tube, one inside the opposite ovary, and a fibroid on an interior muscle of cervix.
I still have 4 more weeks of recovery, but am already feeling the effects of not bleeding every day. That was the goal.
Now, I can start the next chapter of my life without the stress of my (no longer needed) reproductive system trying to do me in.
By the way, I do still have my ovaries. My doctor noted the health benefits of keeping them, such as protecting you from osteoporosis and heart disease.
Plus in my case, and others not yet at that age yet, delaying menopause. Not to mention, there’s no hormone therapy needed if you keep your ovaries.
So, here’s hoping my ovaries stay kind to me for the duration. Otherwise, I am not opposed to doing away with them when necessary.
For now? I’m loving this new chapter!




Looking for more clarity in your life?
Sign up to receive practical tips to start journaling to bring more clarity into your life.